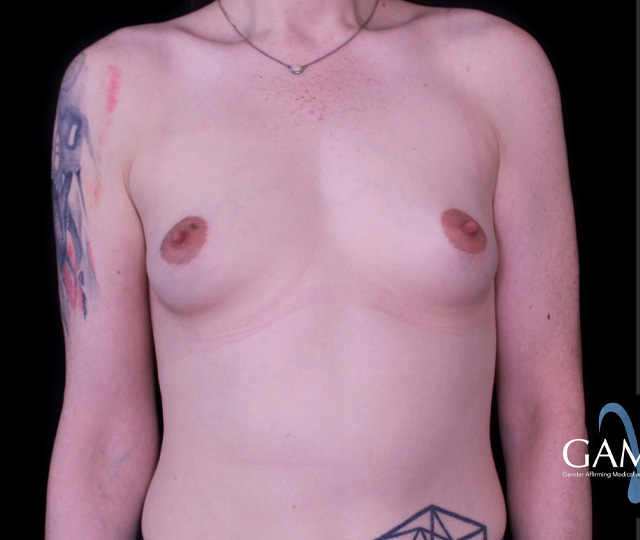
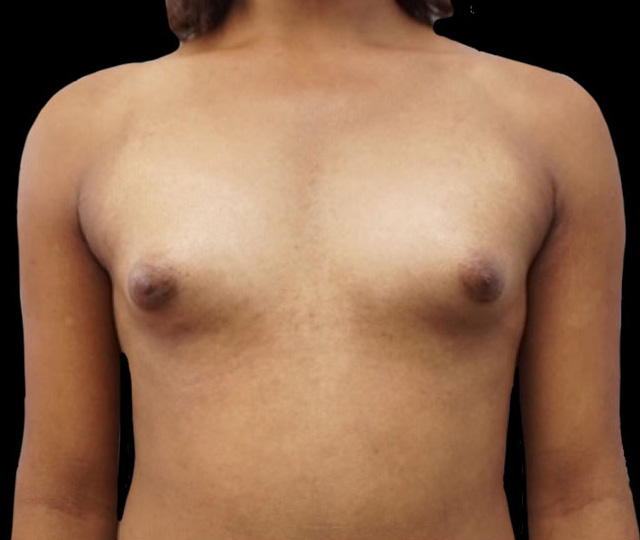
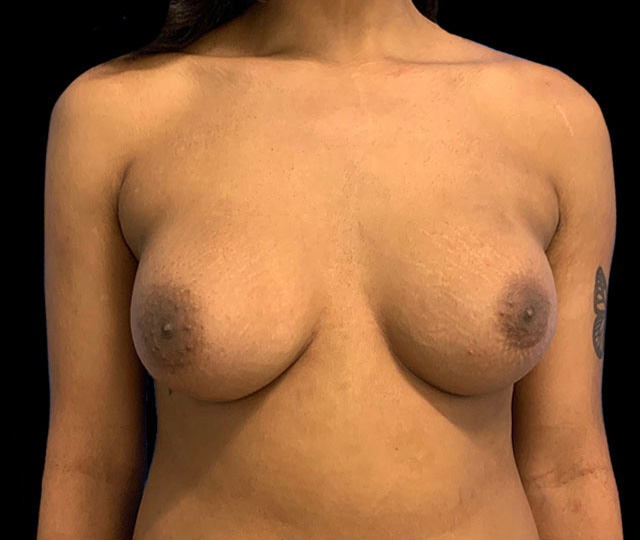
What Is Chest Feminization?
Chest feminization is a gender-affirming surgical procedure designed for transfeminine and nonbinary individuals who wish to achieve a more feminine chest appearance. This surgical procedure, done in both New York City and New Jersey, usually involves placement of a silicone implant underneath glandular tissue and in front of the chest muscle known as the pectoralis. The end goal of this procedure is to create, augment, and shape a natural feminine chest with the desired implant size and shape.
What Are the Different Types of Breast Augmentation?
Dr. Keith and Dr. Marano typically perform chest feminizations with the use of silicone breast implants to augment the chest. Occasionally, fat grafting transferred from elsewhere on the body is injected to shape the chest with or without implants. Dr. Keith and Dr. Marano will discuss the pros and cons of each choice with you in greater depth during your consultation.
Implant-Based Augmentation
For some transwomen, feminization of the chest is achieved through the addition of volume with the use of a breast implant. Typically and most commonly, silicone implants are used to create a feminine chest with natural and desired results. During this procedure, a small incision is made at the inframammary fold at the bottom of the breast to hide the incision. A small pocket is dissected between the glandular tissue and the chest muscle, known as the pectoralis, where the implant will be placed. After placement and confirmation of correct size and position, the incision will be closed with several layers of dissolvable sutures that will prevent the implant from dropping, commonly known as “bottoming out”.
Choosing Implants
At GAMMA, silicone implants are most commonly used for chest feminization procedures. The use of silicone implants over saline implants is preferred, as saline implants may show rippling underneath the chest tissue. At your consultation, a wide array of differently-sized silicone implants will be available for you to try on to determine what best fits your aesthetic goals and desires. The implant size and shape is tailored to each patient based on a series of measurements, unique anatomy, patient goals and preferences, as well as a detailed, joint discussion with Dr. Keith or Dr. Marano about what the best aesthetic results may be for you.
Under Versus Over-The-Muscle Implants
Dr. Keith and Dr. Marano typically employ over-the-muscle – also known as prepectoral – implant placement in transgender females. The reason why placing the implants in front of the pectoralis chest muscle is superior has to do with the negative aesthetic outcomes associated with under-the-muscle (subpectoral) placement. Commonly, when implants are placed under the muscle, they are prone to being squeezed, moved, and visibly distorted when the chest muscle is activated or flexed. This is known as animation deformity. While usually not harmful, animation deformities can potentially increase the risk for implant rupture due to excess squeezing of the implant and create an undesired aesthetic outcome for patients undergoing chest feminization.
Augmentation With Grafted Fat
Dr. Keith or Dr. Marano can perform chest feminization with transferred fat for patients seeking a more subtle chest enhancement. In this case, fat cells are extracted via liposuction from an area of excess fat, such as the stomach, thighs, or flanks. Once they are purified and sterilized, they can be injected into the chest region to create modest but feminine breasts. This procedure, completed in both New York City and New Jersey, also helps to sculpt donor sites. Fat grafting can be completed alone or in conjunction with silicone breast implants for a more natural contour.
Who Are the Best Candidates?
Chest feminization is ideal for patients who desire a natural-looking, feminine chest but have not achieved their full desired outcome through the use of hormone therapy. Patients should be healthy non-smokers with an adequate level of skin elasticity. Ideally, patients should be on hormone therapy for at least one year in order to reach stable breast growth prior to chest feminization with implants. Lastly, they should have realistic yet positive expectations for their results based on their consultation with Dr. Keith and Dr. Marano in New York City and New Jersey.
How Should I Prepare for Breast Augmentation?
Preparing for chest feminization with Dr. Keith or Dr. Marano requires careful planning and steps. Taking the following steps will help ensure your treatment process is seamless and stress-free:
- Provide Mental Health Letter – Many insurance providers and surgical guidelines require a letter from a qualified mental health professional confirming a diagnosis of gender dysphoria and the patient’s readiness for surgery. This letter should follow WPATH (World Professional Association for Transgender Health) standards and address the patient’s understanding of the procedure and its implications. Our team will assist in ensuring the proper language is used and the provider is appropriately credentialed. A letter stating stable breast growth achievement while on hormone therapy is also required for certain insurance companies.
- Quit Smoking – Nicotine constricts blood vessels and significantly increases the risk of complications, including poor wound healing, tissue loss, as well as difficulty with intubation at the beginning of surgery. Patients must stop using all nicotine products—including cigarettes, vapes, nicotine patches, and gum—at least 4-6 weeks before and after surgery. If you are an active nicotine smoker, we will ask you to complete a nicotine blood test as part of your preoperative lab panel to optimize wound healing.
- Manage Medications – You may be asked to discontinue certain medications that increase surgical risks ahead of surgery. At your consultation visit, we will discuss these medications in further detail.
- Well-Controlled Medical or Mental Health Issues / Medical Clearance – To ensure a safe surgery and post-operative recovery, all patients will be required to visit their primary care provider for preoperative clearance 3-4 weeks ahead of surgery. Patients with underlying medical conditions such as diabetes, high blood pressure, asthma, or psychiatric conditions should have them well-managed ahead of surgery with additional clearance letters from corresponding specialists. At your consultation, specific medical clearance instructions will be discussed in further detail.
- Bloodwork and EKG – To ensure that you are medically optimized to undergo surgery, we will send you a prescription for basic blood work and an electrocardiogram to be completed within 3-4 weeks ahead of surgery. This can be completed in conjunction with or ahead of your PCP clearance visit.
- BMI Cutoff – There is no strict BMI cutoff for chest feminization at GAMMA. Every patient is evaluated individually, considering overall health and surgical goals rather than BMI alone.
- Insurance Coverage – GAMMA works with various insurance providers to help patients access gender-affirming surgery. Our team assists with insurance verification, prior authorization, and necessary documentation. Patients should check with their insurance carrier regarding coverage criteria, including mental health letters and medical clearance requirements.
- Complete Your Consultation – You will undergo a detailed consultation with Dr. Keith or Dr. Marano to ensure your expectations are realistic and your health supports the treatment process. Preoperative photos and measurements will be taken during your consultation for surgical planning and optimization. Our team will discuss the risks and benefits, recovery and results, of chest feminization surgery.
- Schedule Help – For the first 24 – 48 hours after surgery, a responsible adult will drive you home and assist you with basic chores. You should also prepare your home environment to support your recovery process.
What to Expect On the Day of Surgery
On the day of surgery, patients should arrive at the surgical center or hospital on time and follow preoperative fasting instructions. Here’s what to expect:
- Check-In and Pre-Op Preparation – You will check in at the surgery center or hospital and complete any final paperwork. A nurse will take your vital signs and place an IV for fluids and medications. You will meet with your surgeon for final markings on your chest, which will guide the breast implant placement. An anesthesiologist will discuss general anesthesia and answer any questions before administering sedation.
- During the Surgery – The procedure typically lasts roughly two hours under general anesthesia. The surgeon will make two small incisions in the inframammary folds underneath the breasts that will allow for the implant to be inserted above the pectoralis muscle. The incisions are closed with several layers of dissolvable sutures that will help to keep the implant in place over time. Although you will not have any surgical drains, you will be placed in a surgical bra administered by the surgery center or hospital.
- Post-Op Recovery – After surgery, you will wake up in the recovery area, where nurses will monitor your vitals. You will be wearing a surgical bra to help reduce swelling and support healing of the implants. Once you are stable and alert, you will be discharged the same day with detailed post-operative instructions.
- Leaving the Hospital or Surgery Center – A responsible adult must accompany you home or to your recovery accommodation. You cannot take public transportation or drive yourself. You may feel tired from anesthesia, and mild discomfort is expected. Pain medication will be provided as needed. It is essential to rest, stay hydrated, and follow all aftercare instructions.
Recovery
After chest feminization, recovery time typically varies by patient from several weeks to months. In general, you may expect the following information regarding recovery:
- Pain Management: Approximately one week ahead of your surgery with Dr. Keith or Dr. Marano, our office will send electronic prescriptions to your pharmacy. These medications include pain medications, stool softeners, and an antibiotic. All medications will be clearly marked and labeled with the correct dosage instructions.
- Drains: Use of surgical drains is dependent on your surgeon performing your chest feminization. During your consultation, your surgeon will specifically discuss the use of drains for your procedure.
- Dressings/Showering: Upon leaving the hospital or surgery center, you will be in a hospital-provided surgical bra that will stay on for 48 hours straight after surgery. After 48 hours, you may take the bra off to shower, but the surgical bra will remain on consistently until the 4-6 week postoperative range. Scar care for your inframammary incisions will typically take place after the four week postoperative visit.
- Activity Restrictions: To prevent surgical postoperative complications, your surgeon will ask you to refrain from heavy lifting, reaching overhead, or vigorous exercise for 4-6 weeks after surgery. Light activity will be resumed at the discretion of your surgeon.
- Time Off Work – Many patients will need 2–3 weeks off of work, depending on their job and postoperative recovery period. Jobs requiring heavy physical activity may require a longer recovery period.
- Postoperative Appointments – After your chest feminization surgery, your surgeon will see you back in the office at 1 week, 1 month, 6 months, and 12 months after surgery to monitor your healing process. Postoperative photographs may be taken during these visits to track and record your healing journey. Based on location, we are able to offer virtual check-ins.
Risks and Complications
Although chest feminization is a relatively low-risk surgery in general, there are risks associated with all surgical procedures. The following are some of the risks or complications associated with breast implantation:
- Pain – Postoperative pain is common but manageable with prescribed medications and rest.
- Hematoma – A collection of blood under the skin that may require drainage in the operating room or reabsorption over time.
- Seroma – A buildup of fluid that may need aspiration during follow-up visits.
- Infection – Although the risk of infection is rare, we employ several measures to decrease risk of infection, such as intraoperative antibiotics, antibiotic irrigation of the implant prior to placement, and postoperative antibiotics.
- Wound Separation– Incisions may take time to heal, with a small risk of partial tissue loss or separation of the incision.
- Change in Sensation– Temporary or permanent changes in sensation may occur with placement of breast implants.
- Implant Rupture, Malposition, Capsular Contracture– Over time, silicone implants are at risk for rupturing, changing position in the chest, or forming a scarred capsule that tightens and thickens around the implant, causing pain and potential aesthetic complications. The FDA recommends having an ultrasound or MRI within the first 5-6 years after initial breast implantation, and every 2-3 years thereafter to assess for rupture or change in position.
Insurance Considerations & Requirements
Most insurance carriers require approval letters from a mental health provider detailing your gender dysphoria and stating that you have been on feminizing hormones for at least 12 months with stable breast growth. We will go over insurance guidelines with you during your consultation with your surgeon to help you gather the necessary documentation.
What Sets Us Apart?
Our team at Gender Affirming Medical and Microsurgical Associates (GAMMA) in New York City and New Jersey is known for providing the highest-level care in an affirming environment. We utilize today’s most progressive and cutting-edge techniques to provide the highest level of service possible. Our goal is to help transgender, nonbinary, and gender nonconforming individuals achieve their unique appearance goals and thrive with confidence, security, and peace of mind.
Dr. Drew Marano
Dr. Drew Marano is an accomplished, board- certified, and fellowship-trained plastic and reconstructive surgeon who has devoted his career to the art of gender affirmation surgery. He graduated from Rutgers New Jersey Medical School at the top of his class, receiving AOA honors before embarking on a competitive six-year Integrated Plastic and Reconstructive Surgery Residency at Columbia University/Cornell University in New York City. Following his residency, Dr. Marano was selected as the first-ever Harvard University Complex Gender and Microsurgery Fellow, during which time he underwent advanced training in groundbreaking and innovative surgical techniques. He is a prolific author, researcher, and lecturer who has contributed to over 40 publications and presentations at regional and national meetings. Dr. Marano offers ongoing support for transgender patients as they navigate their unique and rewarding journey of transitioning.
Dr. Jonathan Keith
Dr. Jonathan Keith is a renowned, fellowship-trained, board-certified plastic surgeon known for his progressive approach to microvascular surgery. He is an active member of the World Professional Association for Transgender Health and the founder of the Rutgers Center for Transgender Health. In 2018, Dr. Keith created the first multidisciplinary clinical program for transgender patients in New Jersey and was the first surgeon in the state to perform a female-to-male phalloplasty for gender affirmation. Regarding his extensive educational background, Dr. Keith completed a demanding seven-year residency at the University of Pittsburgh, one of the nation’s most elite and well-regarded plastic surgery training programs. As a testament to his skill and artistry, in 2012, he received the Stephen S. Kroll Fellowship in microsurgery at the University Hospital of Gent, Belgium. Today, Dr. Ketih performs a range of complex and delicate procedures to assist transgender and nonbinary individuals in achieving their ideal appearance, including DIEP flaps for breast reconstruction, vaginoplasty, and phalloplasty.