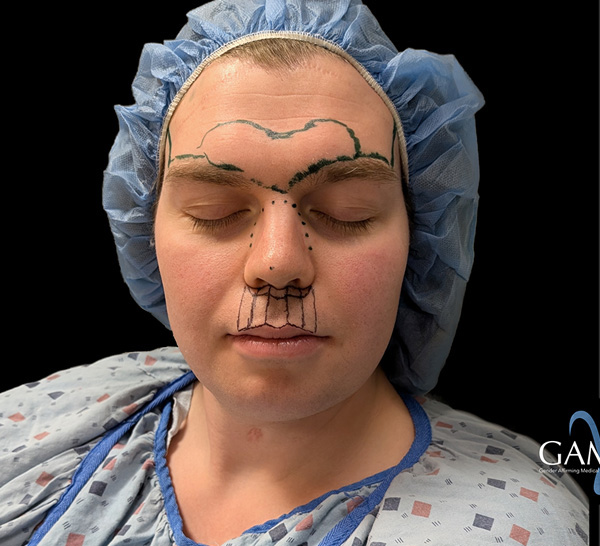
What Is Genioplasty?
Genioplasty is a surgical procedure to reduce and change the appearance of an overly prominent or defined chin, creating a softer, more feminine look in the lower face. Through a series of steps, Dr. Marano and Dr. Keith are able to enhance facial balance by reshaping the chin narrower and softer to achieve a feminine contour. Genioplasty can also correct asymmetry and other contour irregularities.
Surgical Procedure
Genioplasty is performed under general anesthesia and is performed in conjunction with other FFS procedures to optimize feminizing aesthetic results. With genioplasty, the incision is placed intra-orally. By strategically placing the incision inside the mouth along the lower gum, the scar will not be visible on the skin, allows for adequate access to the chin, and therefore provides the best end result.
Once the incision inside the mouth is made, your surgeon will use a customized cutting guide that is jointly designed by your surgeon and biomedical engineers at our partnered medical device team ahead of your surgery. These cutting guides will allow for precision and accuracy when cutting and shaving down the chin to enhance, feminize, and soften the contour of your lower facial shape. Once the necessary cuts are made, the chin is reconstructed into its correct, predetermined position.
Who Are the Best Candidates?
The best candidates for genioplasty are individuals who have a prominent, squared, or widened chin who wish to create a narrower, softer shape. The procedure is also ideal for those looking to improve the overall proportions of facial shape and achieve a more feminine facial aesthetic. A patient’s general health, expectations, and surgical goals will be considered during the consultation to determine the suitability for surgery.
How Should I Prepare for Genioplasty?
The first step in FFS is to meet with Dr. Marano or Dr. Keith for a private consultation at GAMMA in New York City or New Jersey. During this time, you will discuss your goals and medical history with our team, who will then create a customized treatment plan according to your unique anatomy, comfort levels, and goals. Prior to consultation, you should ensure the following:
- Provide Mental Health Letter – Many insurance providers and surgical guidelines require a letter from a qualified mental health professional confirming a diagnosis of gender dysphoria and the patient’s readiness for surgery. This letter should follow WPATH (World Professional Association for Transgender Health) standards and address the patient’s understanding of the procedure and its implications. Our team will assist in ensuring the proper language is used and the provider is appropriately credentialed
- Quit Smoking – Nicotine constricts blood vessels and significantly increases the risk of complications, including poor wound healing and tissue loss. Patients must stop using all nicotine products—including cigarettes, vapes, nicotine patches, and gum—at least 4-6 weeks before and after surgery.
- Manage Medications – You may be asked to discontinue certain medications that increase surgical risks.
- Well-Controlled Medical or Mental Health Issues / Medical Clearance – To ensure safe surgery and recovery, patients with underlying medical conditions such as diabetes, high blood pressure, or psychiatric conditions should have them well-managed. Medical clearance from a primary care provider or specialist is required.
- BMI Cutoff – There is no strict BMI cutoff for FFS at GAMMA. Every patient is evaluated individually, considering overall health and surgical goals rather than BMI alone.
- Insurance Coverage – GAMMA works with various insurance providers to help patients access gender-affirming surgery. Our team assists with insurance verification, prior authorization, and necessary documentation. Patients should check with their insurance carrier regarding coverage criteria, including mental health letters and medical clearance requirements.
- Complete Your Consultation – You will undergo a detailed consultation with Dr. Marano or Dr. Keith to ensure your expectations are realistic and your health supports the treatment process. Our team will discuss the risks and benefits, recovery and results, of FFS.
- CT Scan for Virtual Surgical Planning – Ahead of your facial feminization surgery, your surgeon will provide a prescription for a CT scan of your face. This scan is then used during a surgical planning session with your surgeon and a team of biomedical engineers to create customized cutting guides that allow for extreme precision during your surgery.
What is Virtual Surgical Planning (VSP)?
Virtual Surgical Planning (VSP) is an advanced, cutting-edge technology that allows surgeons to plan facial feminization surgeries with extreme precision and accuracy. This process involves creating a 3D reconstruction of the patient’s facial skeleton, which provides a detailed and accurate representation of the bone structure. Using this 3D model, the surgeon can plan the post-operative bony structure and make decisions about the necessary adjustments.
One of the key benefits of VSP is its ability to provide millimeter-level accuracy in surgical planning, ensuring that the changes made to the facial bones are tailored to the patient’s unique anatomy and desired outcomes. The surgeon uses custom 3D-printed cutting guides and plates, which are created specifically for the patient based on the virtual plan. These guides and plates help the surgeon achieve precise cuts during the procedure, reducing the risk of complications and improving the consistency of results.
VSP is particularly beneficial in complex surgeries, such as genioplasty, where the margins for error are minimal. By using this technology, the surgeon can optimize the approach, anticipate potential issues, and achieve the most aesthetically pleasing and functional outcomes for the patient.
What to Expect On the Day of Surgery
On the day of surgery, you will be given general anesthesia to ensure comfort throughout the procedure. Genioplasty is typically done in conjunction with other FFS procedures. The length of the surgery will depend on what other procedures you are undergoing that day. Once the procedure is complete, you will be closely monitored in a recovery room before being discharged.
Recovery
Recovery times can vary from patient to patient depending on your unique healing abilities, the specific techniques utilized by Dr. Marano and Dr. Keith, and whether any other treatments are performed at the same time. Recovery from genioplasty typically involves a 1-2 night hospital stay if combined with other facial feminization surgeries. Patients can expect to experience some swelling, bruising, and mild discomfort, especially during the first week. A special head dressing and jaw compression garment is worn to support the chin and reduce swelling.
- Activity Restrictions: For 2 to 4 weeks, patients should avoid strenuous activities, including exercise and heavy lifting, to prevent complications.
- Soft Food Diet: As there will be several incisions intra-orally, patients are required to maintain a soft food diet for 2 weeks following surgery. Your surgeon will provide you a list of foods that are acceptable during your hospital stay and while recovering at home.
- Dressings: A hospital-provided jaw compression garment will be worn for 6 weeks after surgery to assist in decreased swelling and optimized contour of the lower facial profile.
- Return to Work: Most patients can return to work after 4 weeks, though it may take longer for complete healing.
- Swelling and Final Results: While swelling and bruising will subside in the first few weeks, final results may take 12-18 months as the chin fully heals and settles into place.
Insurance Considerations & Requirements
Insurance carriers will typically cover gender affirmation surgery, including facial feminization surgery, when it is performed to treat gender dysphoria, a condition in which the patient’s outer traits do not reflect their authentic gender identity. You’ll need a letter from a mental health provider detailing your decision to undergo FFS. Our team can go over the insurance requirements in greater detail during your consultation.
Traveling from Outside the NYC Area
- Resources – For patients traveling to NYC for surgery, GAMMA provides recommendations for LGBTQ+ friendly accommodations, post-op caregivers, and recovery services. Our team can also assist with logistics such as medical transport and aftercare arrangements.
- Requirements – Out-of-town patients must plan to stay in NYC for at least two weeks after surgery to ensure proper healing and attend necessary post-operative appointments. We encourage having a trusted friend, family member, or professional caregiver for the first few days post-surgery.
What Sets Us Apart?
Our team at Gender Affirming Medical and Microsurgical Associates (GAMMA) in New York City and New Jersey is known for providing the highest-level care in an affirming environment. We utilize today’s most progressive and cutting-edge techniques to provide the highest level of service possible. Our goal is to help transgender, nonbinary, and gender nonconforming individuals achieve their unique appearance goals and thrive with confidence, security, and peace of mind.
Dr. Drew Marano
Dr. Drew Marano is a fellowship-trained plastic and reconstructive surgeon who is considered a pioneer in the evolving field of gender affirmation surgery. After graduating at the top of his class with honors from Rutgers New Jersey Medical School, Dr. Marano completed a six-year Integrated Plastic and Reconstructive Surgery Residency at Columbia University/Cornell University in New York City. He was the first-ever Harvard University Complex Gender and Microsurgery Fellow, receiving exhaustive training in today’s most cutting-edge techniques. Dr. Marano is also a prolific author and lecturer and has lent his insights to over 40 publications and presentations at regional and national meetings. He is proud to provide MTF patients with support, encouragement, and life-changing results as they navigate the exciting journey of transitioning.
Dr. Jonathan Keith
Dr. Jonathan Keith is a fellowship-trained and board-certified plastic surgeon known for his consummate skill and artistry in the realm of microvascular surgery. He is a member of the World Professional Association for Transgender Health and the founder of the Rutgers Center for Transgender Health. In 2018, Dr. Keith established the first multidisciplinary clinical program for transgender patients in New Jersey and was the first provider in the state to perform a female-to-male phalloplasty for gender confirmation. He completed a demanding seven-year residency at the University of Pittsburgh, one of the most prestigious plastic surgery training programs in the United States. Today, Dr. Keith is considered one of the most accomplished surgeons in the country who performs DIEP flap surgery for breast reconstruction, vaginoplasty, and phalloplasty.
What Are the Risks Associated with Genioplasty?
The risks and complications of genioplasty may include the following:
- Bleeding: Some bleeding is expected during the procedure, but it is generally controlled with careful surgical techniques.
- Infection: As with any surgical procedure, there is a risk of infection, which can be managed with proper care and antibiotics.
- Numbness: Some temporary numbness in the jaw and lower lip may occur, but it typically resolves over time.
- Swelling and Bruising: These are common side effects following surgery and usually subside within a few weeks.
- Pain: Mild discomfort is common, but it can be managed with prescribed pain medications.
- Mucocele: Formation of a fluid-filled cyst in the oral cavity.
- Bone Resorption: Loss of bone in the area where bone is being cut and removed.